Tech-enabled Urology Medical Billing and Coding Services
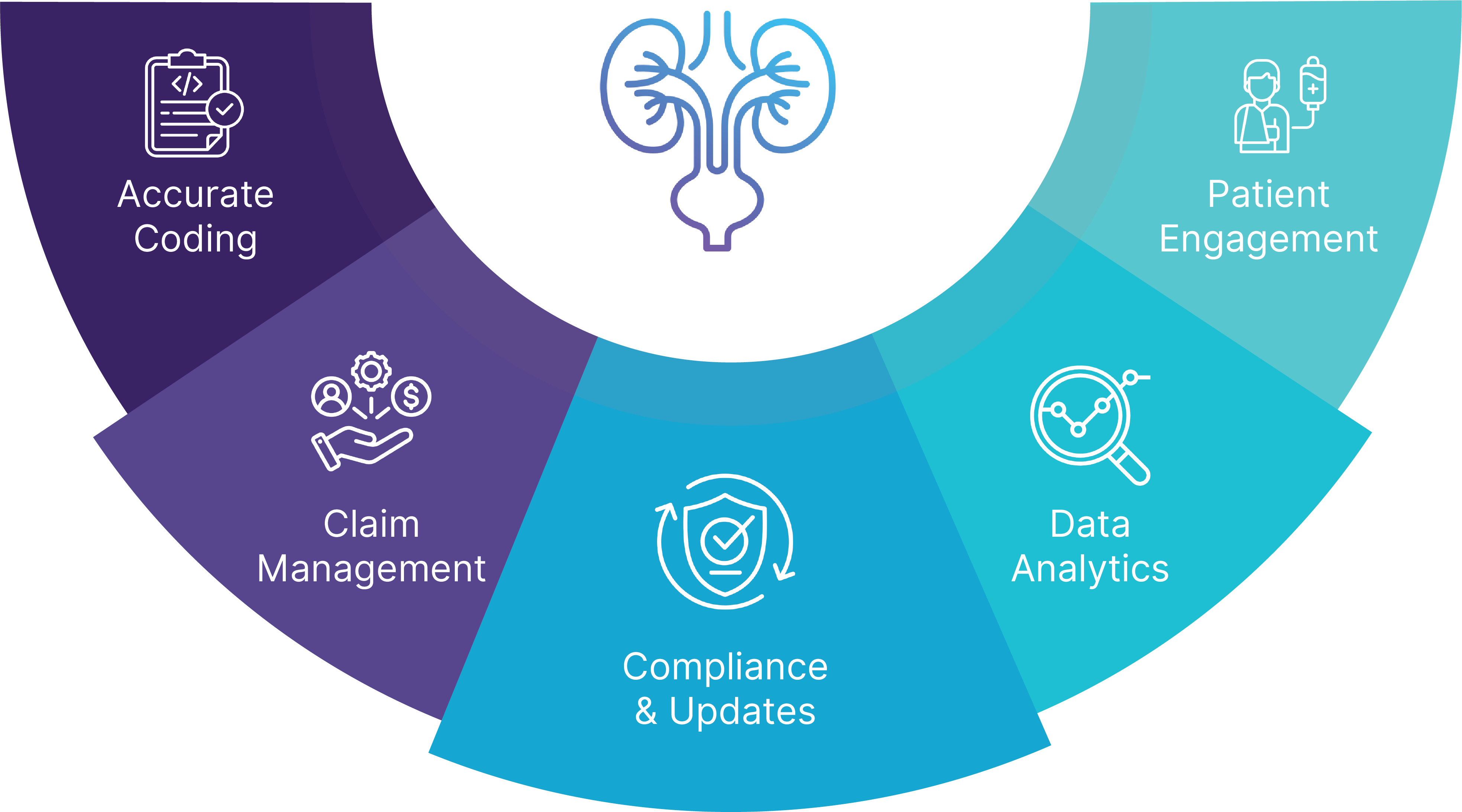
Tech-enabled Urology Medical Billing and Coding Services leverage advanced technology, such as AI-driven coding software, automated claims management systems, and analytics platforms, to streamline the billing process for urology practices. These services include:
Accurate Coding
Tech-enabled Urology Medical Billing and Coding Services leverage advanced technology, such as AI-driven coding software, automated claims management systems, and analytics platforms, to streamline the billing process for urology practices. These services include:
Claim Management
Automating claim submission, tracking, and resolution of denials to enhance cash flow.
Compliance and Updates
Ensuring adherence to the latest regulatory standards (e.g., HIPAA, Medicare, and payer-specific rules).
Data Analytics
Providing insights into revenue trends, claim performance, and operational efficiency for better decision-making.
Patient Engagement
Simplifying patient billing through online portals, automated reminders, and payment options.
Urology Medical Services
These services improve efficiency, reduce errors, and enhance
revenue cycle outcomes for urology practices.
Ascent Health’s Urology Medical Billing Services for Physicians
Ascent Health offers comprehensive, tech-enabled urology billing services designed to meet the unique needs of urologists and their practices. With over 25 years of experience in healthcare revenue cycle management (RCM), we deliver precise, efficient, and compliant billing solutions that allow physicians to focus on patient care while maximizing financial outcomes.
Expertise in Urology Medical Billing Services
Urology involves a wide range of procedures, from diagnostic tests like cystoscopies and urodynamics to advanced treatments such as lithotripsy and prostate surgeries. These procedures require accurate coding and billing to ensure proper reimbursement. Ascent Health’s dedicated team of urology Medical billing specialists is trained in the nuances of CPT, ICD-10, and HCPCS coding specific to urology. This expertise ensures that claims are coded accurately, reducing denials and speeding up reimbursements.
Tailored Solutions for Your Practice

Whether you’re a solo practitioner or part of a large urology group, Ascent Health offers customized solutions to meet your specific needs. Our global delivery centers provide 24/7 support, ensuring your practice runs smoothly around the clock.
Patient-Centric Approach

In addition to optimizing the financial health of your practice, we enhance the patient experience. Our user-friendly patient portals provide clear billing information and flexible payment options, fostering trust and satisfaction among your patients.
Advanced Technology for Efficiency
Our services leverage state-of-the-art technology to streamline the billing process. From AI-driven coding tools that minimize errors to automated claims submission systems, we ensure efficiency and accuracy at every stage. Our analytics platforms provide actionable insights into your practice’s financial performance, helping you make data-driven decisions.
Comprehensive RCM Services
Ascent Health’s urology Medical billing services cover every aspect of the revenue cycle, including:
Eligibility Verification:
Ensuring patients’ insurance coverage is verified before services are rendered.
Coding and Documentation:
Accurate assignment of procedure and diagnosis codes to maximize reimbursement.
Claims Submission:
Prompt and error-free submission of claims to payers.
Denial Management:
Proactive follow-up and resolution of denied or underpaid claims.
Patient Billing:
Simplified patient statements and payment options to enhance collection rates.
Compliance Monitoring:
Adhering to the latest healthcare regulations and payer-specific guidelines.
Case Study – Digital Overhaul Cuts Prior Authorization Time by 15 Days for Urology Network
CPT and ICD Codes Related to Urology Surgeries
Accurate coding is vital for the financial health of urology practices, ensuring appropriate reimbursement while maintaining compliance. Below is an overview of key CPT and ICD codes related to urology surgeries.
Common CPT Codes for Urology Surgeries
50080-50081: Nephrolithotomy procedures.
50590: Lithotripsy, extracorporeal shock wave for kidney stones.
52000: Cystoscopy with bladder irrigation.
52310-52315: Cystoscopy with ureteral stone removal or manipulation.
53440: Urethral suspension procedures for stress incontinence.
55700-55706: Prostate biopsy procedures.
55866: Laparoscopic radical prostatectomy.
57288: Repair of pelvic floor prolapse.
52601: Transurethral resection of the prostate (TURP).
55550: Laparoscopic varicocelectomy.
Common ICD-10 Codes for Urology Conditions
N20.0: Calculus of kidney.
N20.1: Calculus of ureter.
N40.0: Benign prostatic hyperplasia without lower urinary tract symptoms.
R31.0: Gross hematuria.
N13.2: Hydronephrosis with obstruction.
N39.0: Urinary tract infection, site not specified.
C61: Malignant neoplasm of the prostate.
N32.81: Overactive bladder.
N21.1: Calculus in the bladder.
D41.4: Neoplasm of uncertain behavior of the bladder.
Importance of Accurate Coding
Precise use of CPT and ICD codes reduces claim denials, ensures timely reimbursement, and avoids compliance risks. Additionally, proper documentation supporting these codes is essential to justify procedures and treatments.
Partner with Experts
Navigating the complexities of urology coding can be challenging. Partnering with experienced RCM providers like Ascent Health ensures accuracy, efficiency, and adherence to regulatory standards.
For streamlined billing and coding support, trust Ascent Health to optimize your urology practice’s revenue cycle.
Common Billing Challenges for to Urology Surgeries
Urology practices face unique billing challenges due to the complexity of procedures and the intricacies of payer regulations. Addressing these challenges is essential to optimize revenue cycles and maintain compliance. Here are the most common billing issues urology practices encounter:
Complex Coding Requirements
Urology procedures often involve intricate CPT, ICD-10, and HCPCS coding. Missteps in coding, such as incorrect modifier use or improper code combinations, can result in claim denials or underpayments.
Frequent Changes in Regulations
Healthcare regulations and payer policies constantly evolve. Staying updated with changes in Medicare rules, ICD-10 updates, and payer-specific guidelines can be overwhelming for practice staff, leading to compliance risks and revenue loss.
Denials and Rejections
Urology practices often face high denial rates due to insufficient documentation, incorrect coding, or missed pre-authorizations. Managing denied claims effectively requires time and expertise, which can strain practice resources.
Pre-Authorization Complexities
Many urology procedures require pre-authorizations. Failing to secure these approvals in advance can lead to claim rejections. Navigating the pre-authorization process is time-consuming and requires close coordination with payers.
Patient Billing and Collections
High patient financial responsibility, especially for elective procedures, creates challenges in collections. Practices often struggle with communicating billing details, setting up payment plans, or following up on overdue payments.
Technology Integration Issues
Outdated billing systems or a lack of integration between EHR and billing software can lead to errors, inefficiencies, and delays in the revenue cycle.
Addressing These Challenges
Partnering with an experienced RCM provider like Ascent Health can help urology practices overcome these challenges. We offer:
- Expert coding and denial management services.
- Technology-driven solutions for claim processing and patient engagement.
- Real-time analytics to identify and resolve revenue cycle bottlenecks.
Strategies for Urology Billing and Coding Services
- Pre-Approval Requirement
- Justification of Medical Necessity
- Eligibility Verification
- CLIA Number Validation
- Optimizing Coding for Maximum Benefits
- Non-Covered Services
- Billing Restrictions for Certain CPTs
- Utilizing Modifier 59
- Adherence to LCD Guidelines
Pre-Approval Requirement
Ensure prior authorization is obtained for procedures or services that need approval before billing, reducing claim denials.
Justification of Medical Necessity
Provide clear documentation of medical necessity for procedures to avoid denied claims and ensure reimbursement.
Eligibility Verification
Verify patient eligibility for insurance coverage before services are rendered, minimizing billing issues and payment delays.
CLIA Number Validation
Confirm Clinical Laboratory Improvement Amendments (CLIA) certification for laboratory tests, ensuring compliance with regulations and preventing claim denials.
Optimizing Coding for Maximum Benefits
Use accurate and specific codes to reflect procedures, optimizing reimbursements and avoiding undercoding or overcoding.
Non-Covered Services
Identify non-covered services before billing to inform patients and avoid costly denials from insurance providers.
Billing Restrictions for Certain CPTs
Be aware of special billing restrictions for specific Current Procedural Terminology (CPT) codes to avoid errors and payment delays.
Utilizing Modifier 59
Use Modifier 59 appropriately to indicate distinct procedural services, helping to avoid bundling issues and ensuring correct reimbursement.
Adherence to LCD Guidelines
Follow Local Coverage Determination (LCD) guidelines to ensure that claims comply with payer-specific coverage criteria and improve claim approval rates.
Why Choose Ascent Health for Your Urology RCM Needs?
Expertise in Urology RCM
Tech-Driven Solutions
Regulatory Compliance
Dedicated Urology Team
Enhanced Patient Experience
Global Delivery Excellence

With over 20 years of experience, Ascent Health specializes in handling the unique complexities of urology billing and coding services, ensuring maximum reimbursement.
Conclusion
Urology billing services play a crucial role in optimizing revenue by ensuring accurate coding, adherence to insurance requirements, and minimizing claim denials. By focusing on key strategies such as pre-approval requirements, eligibility verification, and the use of appropriate modifiers, urology practices can streamline their revenue cycle management.
